The Condition
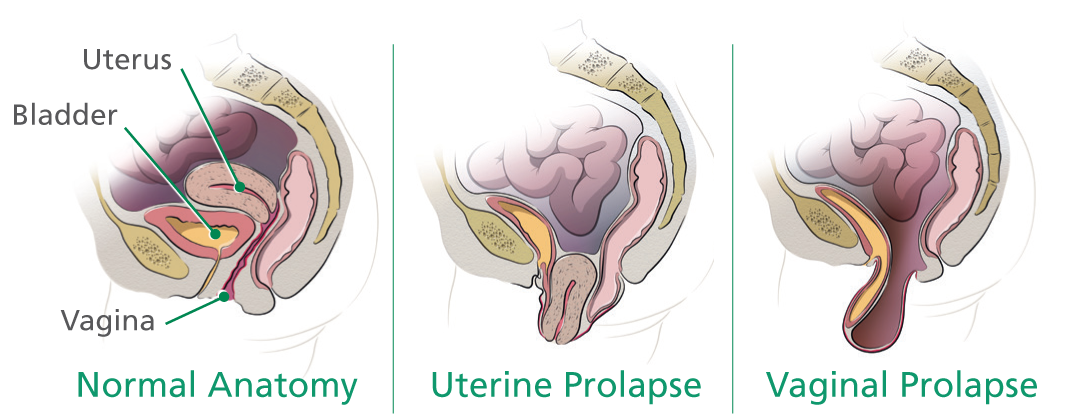
Pelvic prolapse is a condition that occurs when muscles and ligaments supporting your pelvic organs weaken. As a result, these organs (uterus, vagina, cervix, bladder, urethra, or rectum) slip from their normal position.
Severe uterine prolapse can cause the uterus to slip partially into the vagina. It may cause the upper part of the vagina to sag into the vaginal canal or even outside the vagina.
Some women with prolapse have no symptoms. Others may experience: a feeling of sitting on a
ball, pulling in the pelvis, pelvic or abdominal pain, painful intercourse, protrusion of tissue from the vagina, bladder infections, vaginal bleeding, unusual discharge, constipation or frequent urination.
Pelvic prolapse is common, affecting about one in every three women who have had a child. One in nine women experience symptoms severe enough to need surgery. Risk factors for prolapse include multiple vaginal deliveries, age, obesity, hysterectomy and smoking.
Surgery Options: Sacrocolpopexy
Your doctor may recommend medication or lifestyle changes to ease your symptoms. If non-surgical treatments do not help or if your symptoms get worse, your doctor may recommend surgery. The procedure is called sacrocolpopexy. During the operation, surgical mesh is used to hold your affected pelvic organ(s) in their natural position. The mesh remains in place permanently. This procedure is
not the same as what occurs during transvaginal placement of mesh. Your doctor can fully explain the differences and process to you.
Sacrocolpopexy is considered the most effective way to correct pelvic prolapse and resolve symptoms. It may also be performed following a hysterectomy to provide long-term support of the vagina.
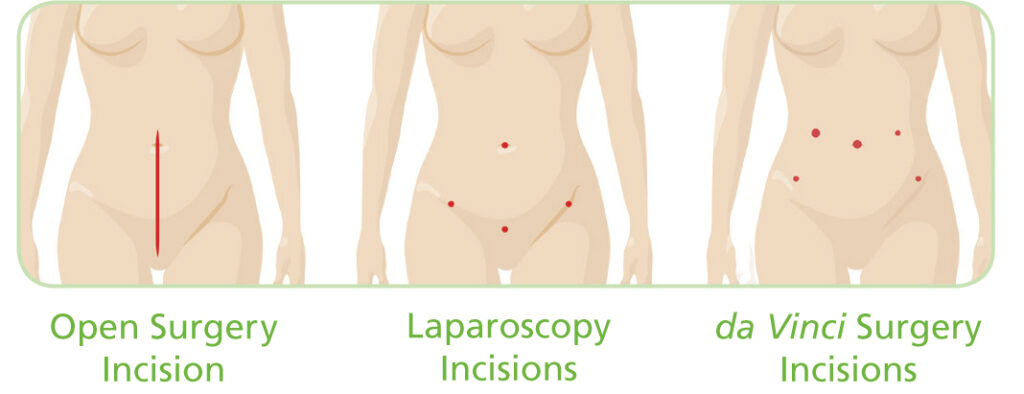
Sacrocolpopexy has traditionally been performed using open surgery. A long, horizontal incision is made in the lower abdomen which allows doctors to reach your pelvic organs.
Laparoscopic surgery is a minimally invasive alternative to open surgery. With laparoscopy, your surgeon operates through a few small incisions using a tiny camera and long, thin surgical instruments. The camera sends images to a video monitor in the operating room to guide surgeons as they operate.
Another minimally invasive surgical option for women diagnosed with pelvic prolapse is da Vinci Surgery.
da Vinci Surgery: A Minimally Invasive Surgical Option
With da Vinci, surgeons operate through a few small incisions – similar to traditional laparoscopy. The da Vinci System features a magnified 3D HD vision system and wristed instruments that rotate far greater than the human wrist. These features enable surgeons to operate with enhanced vision, precision, dexterity and control.
As a result of da Vinci technology, da Vinci Sacrocolpopexy offers the following potential benefits over open surgery:
• Less blood loss
• Shorter hospital stay
• Small incisions for minimal scarring
As a result of da Vinci technology, da Vinci Sacrocolpopexy offers the following potential benefits compared to traditional laparoscopy:
• Shorter operation
• Less blood loss
• Shorter duration with catheter
Additional potential benefits of da Vinci Sacrocolpopexy:
• Low rate of complications
• High sexual function
• Improved urinary, bowel and pelvic symptoms
Patient Testimonials
The Enabling Technology: da Vinci Surgical System
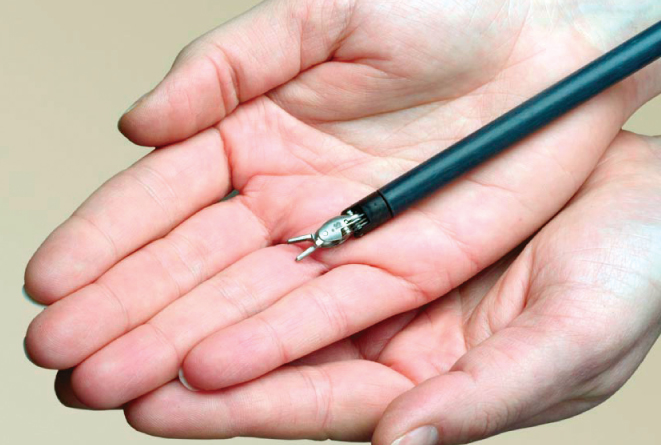
The da Vinci Surgical System is designed to provide surgeons with enhanced capabilities, including high- definition 3D vision and a magnified view. Your doctor controls the da Vinci System, which translates his or her hand movements into smaller, more precise movements of tiny instruments inside your body.
Though it is often called a “robot,” da Vinci cannot act on its own. Surgery is performed entirely by your doctor. Together, da Vinci technology allows your doctor to perform routine and complex procedures through just a few small openings, similar to traditional laparoscopy.
The da Vinci System has been used successfully worldwide in approximately 1.5 million various surgical procedures to date. da Vinci – changing the experience of surgery for people around the world.
Content provided by Intuitive Surgical.